Ketamine Infusion Therapy For Depression – How Does it Work?
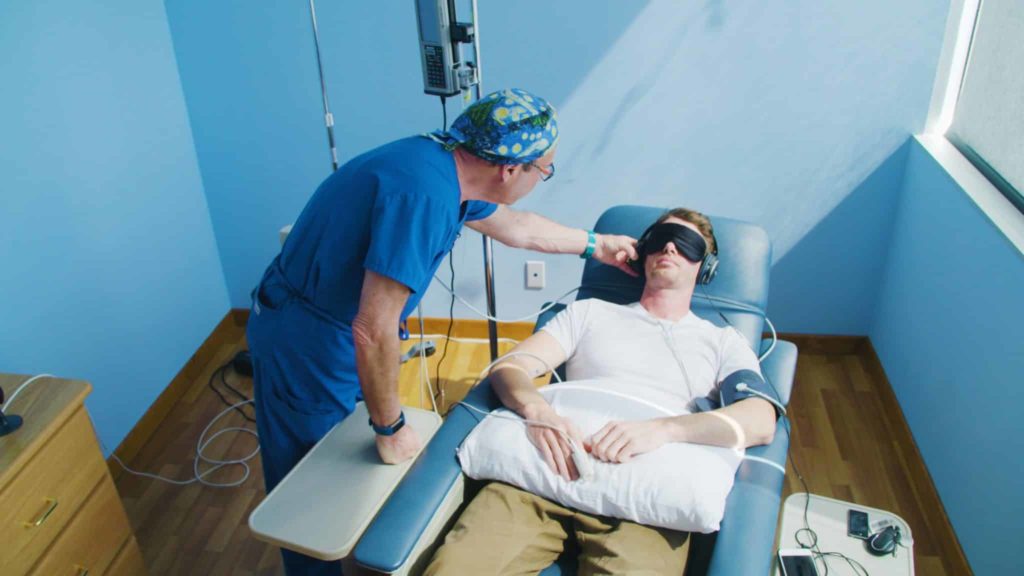
In the medical world, an infusion is the therapeutic introduction of a fluid other than blood to the human body, by way of the vein and straight into the patient’s bloodstream. Such fluids may include saline (salt) solutions, chemotherapeutic or non-chemotherapeutic agents, or in the case we shall discuss below, a ketamine solution.
Whilst injections are also a way of introducing solutions to a patient’s bloodstream by way of the vein, the sole differentiator between an injection and an infusion is the amount of time required for the solution to fully enter the patient’s bloodstream. If the process of transferring the fluid (usually in solution form) into the bloodstream takes less than fifteen minutes, it is an injection. If it takes more than fifteen minutes, it is an infusion.
Ketamine For Depression
Evidence that is growing more expansive by the day is highlighting ketamine as a powerful solution for depression – even in the worst of treatment-resistant cases. Ketamine is a powerful general anesthetic which stops feelings of pain, and it’s used for the carrying out of operations on both humans and animals. The effects are fairly short-term, but until they do fade, ketamine may cause a loss of physical sensations in the body and sometimes patients experience muscle paralysis. It can also lead human beings to experience a distortion in their perceived reality.
Other recent studies have also shown that ketamine has demonstrated significant promise as a rapidly-acting antidepressant in treatment-resistant patients with unipolar MDD. On top of this, the ever-expanding evidence is now also demonstrating that ketamine may be efficacious also in patients with bipolar depression, post-traumatic stress disorder (PTSD), and acute suicidal ideation.
How Do We Usually Deal With Depression?
Treatments for depression are usually decided based on the severity of the case in question. For milder cases, doctors may instruct patients to ‘wait and see’ what happens to their symptoms or to get out and exercise more. They may also suggest a level of self-help, by way of accessing local mental health-focused groups in their area, or by accessing online Cognitive Behavioral Therapy (CBT) communities or even by reading self-help books based around the topics of mental health and depression.
For mild to moderate cases, talking therapies are the most common treatment focus. For example, Cognitive Behavioral Therapy and/or counseling. But when we look at more severe symptoms, the first treatment method to which health practitioners turn is usually an antidepressant drug. There is a total of thirty different types of antidepressant and they must be prescribed by a practitioner sufficiently qualified to make the relevant diagnosis of depression, as well as determining whether or not the symptoms are severe enough to have antidepressants prescribed in the first place.
The issue with antidepressant routes to the treatment of depression, especially when considering symptoms of a more severe nature, is that there is an increasing number of clinical cases that are proving to be resistant to the more ‘traditional’ antidepressant treatments. This is even the case when combined with other treatments, such as psychotherapy and other more holistic, complementary forms of therapy. Generally (in the UK), an adequate treatment trial lasts from 6-8 weeks, and a clinical case of depression isn’t generally defined as treatment-resistant until after foregoing at least two antidepressant trials. This clearly demonstrates that a lapse of considerable amounts of time is required to determine whether or not the treatment a patient receives is having an adequate effect. And the consequences of prolonged severe symptoms of depression that have proven to be treatment-resistant can become quite worrying. This is the exact gap that ketamine appears to be filling in recent times.
A New Concept; Superior Results
Ketamine has been used for the treatment of pain since the 1960s when it was used to operate on soldiers during the Vietnam War. However, research and trials utilizing ketamine for depression and mood alterations are much more modern. Researchers began studying ketamine from this perspective in the year 2000, and since then it has proven to improve mood states much quicker than traditional antidepressant drugs, and it even works when some of these other drugs have failed.
Research since 2006 on the use of ketamine for treating depression has shown that subanesthetic doses (0.5 mg/kg) administered over a 40-min intravenous (IV) infusion period can have rapid-acting antidepressant effects on patients with TRD. The presumed mechanisms of the antidepressant effects of ketamine involve activating synaptic plasticity by increasing brain-derived neurotrophic factor (BDNF) translation and secretion, as well as via glycogen synthase kinase-3 (GSK-3) inhibition. BDNF is also associated with behavioral responses to classical antidepressants. Whereas it takes several weeks for BDNF-mediated synaptic plasticity triggered by standard antidepressants, such synaptic plasticity changes seem to occur in a matter of hours after administration of ketamine. And it appears that the intravenous route of administration is the most effective of all.
But Why Intravenous (IV) Ketamine, Specifically?
Ketamine could be administered in a variety of ways – namely as an intravenous infusion, as an intramuscular injection, or as an intranasal spray. But why is the IV route proving to be overall the most popular route of administration? It’s to do with a thing called bioavailability. This refers to the amount of the administered solution that is actually available for the body. How much of the solution the body is able to see and utilize. I.e. the active portion of the solution that actually reaches your bloodstream and is able to treat what is bothering you. And the rest of the solution? It is either altered, digested, excreted, or discarded in some other way by your body.
IV administration of ketamine is the one and only route of administration that guarantees 100% of the ketamine being available for your body and thus 100% of it reaching your brain, which is exactly where it needs to be. This may leave you asking how exactly a patient’s exact dosage is calculated, to ensure the correct amount is being administered during any given treatment.
The dosage of a ketamine infusion treatment is calculated based on the patient’s body weight on the specific day of treatment and broken down to a tenth of a milligram. After this, it is mixed with relevant amounts of saline solution (sodium chloride and water) before it is slowly ‘infused’ directly into the patient’s bloodstream, similar to how fluid is given to someone who is dehydrated.
When using an infusion as the route of ketamine treatment for depression, there are zero obstacles preventing the solution’s perfect entry into the patient’s bloodstream and thus its arrival directly to their brain. This is something that anesthesiologist have known for some decades now. Therefore, some may argue that ketamine was, quite literally, designed to be given intravenously.
An Unclear Future, But A Definite Rapid-Acting Treatment
Unfortunately, ketamine has also proven to be ‘one of those’ drugs able to be hijacked for illicit experiences. If ketamine is made available to patients via nasal sprays to be used on an ‘as needed’ basis, this significantly increases the risk of the solution being administered improperly, being abused or even sold illegally on the streets. This makes it clear that the IV route of ketamine administration is, without doubt, the best and most reliable approach out there.
There is still a significant gulf in conclusive research surrounding the long-term efficacy of ketamine as a treatment for depression. The psychotomimetic properties may indeed, at least to some extent, complicate the application of this pharmacological agent. However, despite the fact that many further studies are required to evaluate its long-term antidepressant efficacy, ketamine may definitely be considered a valid and intriguing antidepressant option for the treatment of TRD.